FIRST AID
IF YOU HAVE BEEN BITTEN CALL 000 AND IMMEDIATELY APPLY A PRESSURE BANDAGE TO THE EFFECTED LIMB.
NOTE: All snake bites should be treated as venomous especially in the absence of reliable identification and first aid action should be applied immediately.
The following information is a guide of what TO do and what NOT to do in the event of a snake bite.
1. Call 000
2. Calm the bite victim, stop them from moving (moving spreads the venom faster)
3. Apply a pressure bandage using the “Pressure Immobilisation Technique” or PIT. Note: If
resuscitation is needed it takes precedence over the PIT. However PIT should be applied
as soon as possible to potentially minimise further venom flow.
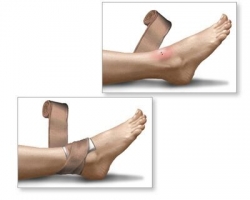
4. For bites on a limb, apply a broad pressure bandage over the bite site as soon as
possible. Elasticised bandages (10-15cm wide) are preferred over crepe bandages, if neither are available, clothing or other material should be used. The bandage should be firm and tight, you should be unable to easily slide a finger between the bandage and the skin.
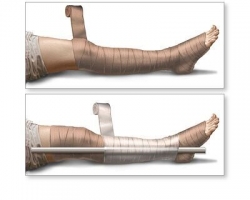
5. In order to further restrict lymphatic flow and to assist in immobilisation of the limb, apply a further pressure bandage, commencing at the fingers or toes of the bitten limb and extending upward covering as much of the limb as possible. The bandage should be applied over existing clothing if possible. The purpose of this bandage is to further restrict lymphatic flow and assist immobilisation. (Alternatively, a single bandage may be used to achieve both pressure on the bite site and immobilisation of the limb. In this method, the bandage is initially applied to the fingers or toes and extended up the limb as far as possible including the bite site).
6. Splint the limb including joints on either side of the bite, to restrict limb movement. The splint material can be incorporated under the layers of the bandage. For the upper limb, use a sling.
7. Keep the victim and the limb completely at rest. Bring transport to the victim if possible. Transport the victim to medical care, preferably by ambulance. If alone, the victim should apply the pressure immobilisation bandage as completely as possible over the bite site and affected limb. They should keep immobile until assistance arrives. If they are unable to obtain urgent help to come to them, then apply local pressure (if possible) and move themselves to seek urgent help. Do not remove the bandages or splints before evaluation in an appropriate hospital environment.
8. If the bite is not on the limb, firm direct pressure on the bite site may be useful. Do not restrict breathing or chest movement and do not apply firm pressure to the neck or head.
- DO NOT cut the bitten area, or attempt to suck venom from the bite site.
- DO NOT wash the bitten area (If anti-venom is required hospitals need to swab the area for traces of venom to test which type of anti-venom to use)
- DO NOT apply an arterial tourniquet. (Arterial tourniquets that cut off circulation to the limb, are potentially dangerous and are not recommended for any type of bite or sting in Australia)
- DO NOT remove the bandages or splints at any stage after they are applied. Only with medical support under direction of a treating doctor should bandages be removed. Further, Only when appropriate antivenom and resuscitation equipment is on hand, should medical staff remove any first aid.
- DO NOT unnecessarily move the bite victim. Application of first aid should be done as soon as the bite is received or when first noticed. Again unnecessary movement results in the venom moving through the system faster.
- DO NOT give food or drink - In the event of significant delay or if dehydration is an issue, small sips of water are acceptable. Alcohol especially should be avoided.
Recognising a bite (Signs & Symptoms)
The bite may be painless and without visible marks. Other symptoms and signs may include:
- Paired fang marks, but often only a single mark or a scratch mark may be present (Localised redness and bruising are uncommon in Australian snakebite) Headache
- Nausea and vomiting
- Occasionally, initial collapse or confusion followed by partial or complete recovery Abdominal pain
- Blurred or double vision, or drooping eyelids
- Difficulty in speaking, swallowing or breathing
- Swollen tender glands in the groin or armpit of the bitten limb Limb weakness or paralysis
- Respiratory weakness or respiratory arrest.
Life-threatening effects may not be seen for hours. However when massive envenomation occurs, especially in children, symptoms and signs may appear within minutes.
Disclosure: Used in this guide is information from the AUSTRALIAN RESUSCITATION COUNCIL (GUIDELINE 9.4.1). They are the leading authority on first aid treatment in Australia. The information presented on this website is offered as a guide only and should not be substituted for a nationally recognised first aid certificate.

First Aid PDF - Click Icon Below:







